What Causes Morgellons Disease: Understanding Borrelia Spirochetes
Imagine you hire armed security guards because you just attained a priceless piece of art. No one likes the thought of a cat burglar breaking in past the security guards and making away with the art without being caught.
But this may be just what’s happening within the immune system of Morgellons patients trying to deal with the unwanted intruder of Borrelia burgdorferi spirochetes. The security system is simply outmatched by a smaller, faster opponent. And that leaves the priceless artifact of good health in the hands of the invaders.
Through this article, we’ll explain how Morgellons patients suffer from a low-level, persistent infection rather than a mental illness many claim. Despite having many avenues for testing, Morgellons patients and their doctors often come up short when diagnosing this debilitating disease.
By piecing together the latest research around Borrelia burgdorferi, a tick-borne pathogen, the Charles E. Holman Morgellons Disease Foundation would like to help you better understand spirochetal infections and Morgellons disease.
What is Borrelia burgdorferi?
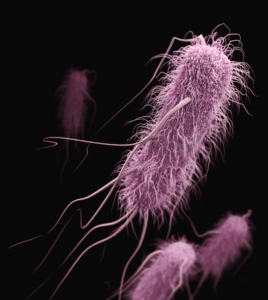
Example of flagellated bacteria
Through many scientific and clinical evaluations, researchers have noted that up to 98% of Morgellons patients have tested positive for Borrelia burgdorferi infections—the leading player in Lyme disease.
Borrelia burgdorferi (Bb) is a flagellated spiral-shaped bacteria or spirochete that has many tails. The bacterium uses these tails as tiny propellers to swim through fluids. Bb colonies can be found in small rodents and spread to new hosts through bites from the blacklegged tick—a prominent tick species across much of North America.
Ticks feast on many different hosts—including humans—throughout their life cycle, transmitting the infecting bacteria during each blood meal. Bb primarily lives in the tick’s gut, but when conditions are right, it migrates up the tick, collecting in its saliva and spreading to the new host.
Once in the new host, Bb quickly colonizes host tissues. The groups of growing and dividing bacteria depend on host cells like human skin cells to provide the nutrients they need to survive.
How Borrelia burgdorferi spreads through the body
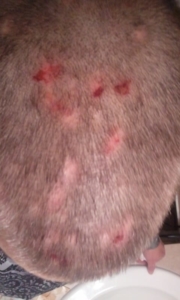
Morgellons Disease on Scalp
If left untreated, the founding colony of fully motile or swimming bacteria quickly disseminates through the host’s tissues. In regards to human patients, this means that the infection can spread throughout the body and into other tissues—not just skin—causing the vast array of symptoms we see in Morgellons and Lyme disease patients.
Spirochetes are up to one thousand times smaller than the cells that make up our bodies. The size disparity, paired with their high motility, allows them to swim through our dense tissues, cellular structures, and membranes.
Usually, our immune system does a fabulous job catching and eliminating invasive bacterial threats. However, natural immune system response isn’t up to the chase for many patients. Human immune cells can only travel through the extracellular space—the fluid surrounding individual cells in tissues. They’re too large to fight infection inside individual tissue cells where Bb can hide.
Special adaptations like its slender body shape, minuscule size, and high mobility allow Bb to enter cells, outmaneuver immune responses and travel through the host tissues without using the bloodstream. As Bb infection spreads throughout the body, the types of lesions left in its wake reflect the progressive stages of the disease.
Treating Borrelia burgdorferi infections
Borrelia burgdorferi spirochetes are the ultimate cat burglars of the cellular world, as we alluded to above. Not only can they outrun immune cells, but Bb can also evade many forms of clinical testing and antibiotic treatments.
Borrelia spirochetes have an entire repertoire of adaptations that allow them to survive adverse conditions. Some antibiotic treatments, like doxycycline, azithromycin, and nitazoxanide work by collecting in the extracellular space—creating harmful conditions and preventing growth. In the presence of these medications, the bacteria can turn on genes that will slow growth or change into a cyst.
In cyst form, Borrelia species can survive almost indefinitely in poor conditions. When the environment improves, cysts will revert back into spirochetal form and proceed to colonize within the host tissues. This behavior could explain why many Morgellons patients find relief through antibiotic therapy, but experience flare-ups after treatment stops.
Many medications used to treat bacterial infections cannot pass through cell walls and enter intracellular spaces within tissues. The spirochetes may improve their survival by slipping through cell walls and hiding inside the host’s cells—where antibiotic drugs cannot reach them.
Limits of Borrelia burgdorferi testing
While it’s true that a Borrelia infection may seem bloodborne—it is spread by a tick after all—this isn’t the case. In reality, Borrelia species don’t spread through the body via the host’s bloodstream. It doesn’t need to since it can swim through tissues. Knowing this, it makes sense that patient blood tests often come back negative, spurring many medical professionals to say Morgellons is a mental disorder rather than a biological malady.
But there’s more than one way to use blood testing to diagnose disease.
Even though the pathogen doesn’t travel through the bloodstream, the markers a host’s immune system uses to hunt spirochetes do. Scientists can identify these markers called antibodies in a patient’s blood sample and count how many there are. The antibody count will be high if the patient is fighting an ongoing infection. The antibody count will decrease as the immune system conquers the infection and clears the pathogen.
While this may seem straightforward, Borrelia’s adaptations discussed above come into play. If the spirochetes have gone dormant or become cysts, the immune system may not be making antibodies against them. That means even serological antibody testing can lead to false negatives.
Cultures and PCR
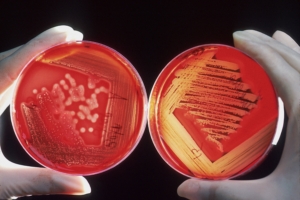
Example of cell culture growth
Scientists can also take tissue samples, grow bacterial cultures, or test for Borrelia DNA. While growing cultures can be an accurate testing option, the growth and identification process may be not only lengthy but expensive.
DNA testing may not always be accurate as the lab-grown strains of Borrelia spirochetes are genetically different from the strains found in the wild, which may also account for false-negative test results leading to harmful misdiagnosis.
Light microscopy
Due to these constraints, light microscopy is one of the best ways to diagnose Morgellons disease clinically. Using a handheld microscope, clinicians can examine lesions for colored Morgellons fibers. While how the spirochetal infection triggers fiber production is still unknown, they seem to be caused by Borrelia spirochetes hiding in specific skin cells.
Borrelia burgdorferi and Morgellons disease
While it is true that the vast majority of Morgellons patients have experienced an underlying Borrelia burgdorferi infection, researchers still don’t fully understand the infection’s mechanics in Morgellons patients.
Many questions remain as to whether Morgellons symptoms are, in fact, due to a persistent infection, a reaction with dead spirochetes, an autoimmune disease triggered by an initial infection, or all of the above.
We know Morgellons disease has a pathogenic cause—it’s not a delusional disorder. Morgellons patient suffering is real, tangible, and can be successfully treated with the right approach.
Through your charitable donations, the Charles E. Holman Morgellons Disease Foundation can help fund future studies to find answers for those suffering.
Every little bit counts. Please consider donating $5 or more to help relieve the suffering of future Morgellons patients.

