Understanding Morgellons Arthritis
Morgellons disease’s hallmark symptoms include widespread slow-healing open sores and unusual-colored filaments found in the skin or protruding from lesions. However, the disease attacks a number of body systems, leading to an array of other difficult symptoms including overwhelming fatigue, muscle aches, heart problems, digestive issues, brain fog, and joint pain.
Through this article, The Charles E. Holman Morgellons Disease Foundation would like to raise awareness of how the underlying bacterial infection affects patients’ joints and connective tissues.
Spirochetal spread
 Morgellons disease is a tick-borne illness caused by the same bacteria responsible for Lyme disease. For unknown reasons, roughly 6 percent of Lyme patients develop Morgellons disease and middle-aged caucasian women seem to be affected more frequently.
Morgellons disease is a tick-borne illness caused by the same bacteria responsible for Lyme disease. For unknown reasons, roughly 6 percent of Lyme patients develop Morgellons disease and middle-aged caucasian women seem to be affected more frequently.
Severe physical symptoms caused by this disease often sideline patients from their own lives as they compound pre-existing insecurities like anxiety and mood disorders. The mental anguish they suffer is often incalculable.
Morgellons disease spreads through black-legged tick bites. Borrelia burgdorferi, a spirochetal bacteria, is carried by the tick and infects unsuspecting human hosts.
After a bite, some people develop erythema migrans, a bullseye rash, and a tell-tale sign of infection. Other victims may not manifest a typical rash or any rash at all and may not know they’re infected until they have symptoms many months or even years after a tick encounter.
Because early infection symptoms aren’t overly specific, both patients and healthcare providers often flail while trying to pinpoint a cause. The lack of easy diagnosis means many patients miss getting early intervention, allowing the infection to spread throughout their bodies. This allows Morgellons skin lesions to later manifest.
The infecting bacteria, Borrelia burgdorferi, is classified as a spirochete. It has a slender body many times smaller than human cells. In addition to other adaptations, this spirochete can swim through dense tissues and between cell walls to escape immune system counterattacks.
After initial infection, spirochetes replicate and grow near the bite site before using their particular adaptations to travel or disseminate throughout the patient’s body.
The bacterial infection will spread to colonize faraway tissues like the heart, nervous system, and joints. As the spirochetes spread, the patient’s immune cells trigger an inflammatory response that will continue in areas where the bacteria invade.
Inflammation
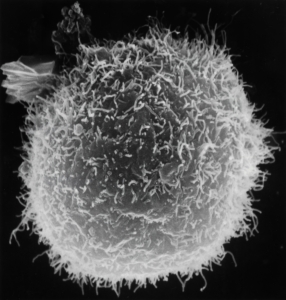
Example of a white blood cell
Generally, our bodies use inflammation to increase blood flow to an area bothered by an irritant. Increased blood flow brings more white blood cells that can help fight the invading spirochetes. While it serves a purpose, inflammation can also trigger redness, heat, swelling, pain, loss of function, and even a fever.
Compounding the problem, battling an infection takes enormous energy. That means patients will likely feel persistently sick, drained, and feverish. That leaves many Morgellons patients with little energy to live their everyday lives.
Morgellons arthritis
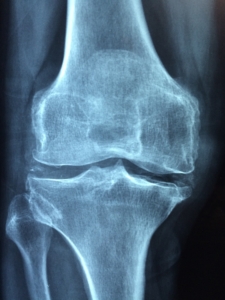
When the bacteria reach large joints, such as a patient’s knees, spirochetes invade the joint tissues, triggering a localized inflammatory response.
As a result, patients’ knees will visibly swell and often be red-hot to the touch. Excessive swelling can tear connective tissues, causing lesions throughout the joint. Knee swelling can become so severe that Morgellons patients are unable to walk.
Patients may experience consistent joint swelling or suffer from “attacks” that come and go for several months or, in extreme cases, many years.
 Often, for patients who are diagnosed with Lyme shortly after becoming infected, a four-week course of antibiotic therapy can kill the invading bacteria and rid a patient of their underlying infection.
Often, for patients who are diagnosed with Lyme shortly after becoming infected, a four-week course of antibiotic therapy can kill the invading bacteria and rid a patient of their underlying infection.
However, antibiotics may fail to stop the infection and alleviate symptoms for many Morgellons patients. As the underlying Borrelia burgdorferi infection persists, so does the patient’s inflammation and Morgellon’s symptoms linger.
Researchers have found that Borrelia burgdorferi spirochetes may persist or hide from antibiotics and immune cells for over six months after being treated for Lyme disease, leading to a Post Treatment Lyme Disease Syndrome (PTLDS) diagnosis.
In other instances, research shows that certain particles shed by growing spirochetes can cause an extreme inflammatory response.
In this study, researchers injected mice with specific bits of cell-wall material from Borrelia burgdorferi spirochetes. The mice experienced extreme joint swelling almost immediately. Throughout the course of the study, researchers found that the mice could not clear spirochete particles from their joints and swelling lasted for several months—despite being free of infection.
Evidence suggests that patients’ immune systems may also create antibodies against the particle which can trigger an inflammatory response leading to extreme tissue damage.
These mechanisms may work together to exacerbate joint swelling in infected patients.
No treatment options currently exist that will manage symptoms across the board for Morgellons patients who haven’t had success with antibiotics. Until researchers can pinpoint reproducible treatment options, patients will continue to suffer.
This is where The Charles E. Holman Morgellons Disease Foundation needs your help. Using your donations, we can fund ground-breaking research to help us understand Morgellons disease and find potential cures. We also work closely with grassroots organizations to increase understanding and awareness of this debilitating disease.
Please donate today to allow our researchers to identify novel treatment solutions for Morgellons arthritis and its other symptoms.

